The relationship between resting energy expenditure (REE) (kJ/d) and
body mass (M) (kg) is a cornerstone in the study of energy physiology.
By expressing REE as a function of body mass observed across mammals,
Kleiber (1930) formulated the now classic equation: REE = 293M0.75.
(1). Calder (1984) (2) has shown that such a relationship holds also for
organs in an adult body. The following equation describes the relationship
between organ mass and tissue mass.
T = b * M^q where b is a constant and
q is a scaling exponent
This relationship holds for mammals e.g., mouse or elephant and is called
an allometric law. It is a manifestation of an optimality principle which
controls the structure of organisms. The size of each organ depends on, and
is controlled by the overall size of the body. The whole controls
its parts.
Breast cancer
An important study by Demicheli et al (3) revealed that this law describes
also the relationship between a tumor of the breast and axillary lymph nodes.
The graph published by the team depicts the proportion of patients with positive
lymph nodes as a function of tumor volume in the adjacent breast.
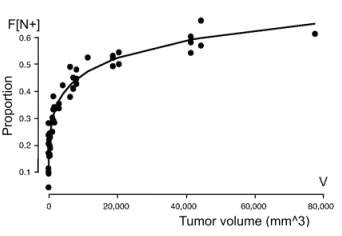 |
The curve is derived from the following equation F[N+] = 1 exp(0.0586
V 0.254) (3)
F[N+] : proportion of positive lymph nodes
V : Tumor volume
The implications are startling.
Axillary lymph node involvement indicates tumor metastasis. Metastatic seeding
depends on tumor size and is non linear. Actually the graph depicts also tumor
evolution whose seeding rate, which is the derivative of F[N+] or
F[N+] is depicted below.
F[N+]. =
Metastasis rate is inversely proportional to tumor size.
The bigger the tumor the slower its rate of metastasis. In other words tumor
controls its metastasis rate. More precisely tumor and metastasis constitute
one system. They are one organ that evolves as a whole.
Metastatic seeding following surgery
Many clinical studies report a metastatic flare up following tumor surgery,
like the appearance of liver metastases following the surgery of colon cancer.
Surgery leads to mobilization of tumor cells into peripheral blood which is
generally attributed to manual tumor handling. Yet the following study on
metastasis following treatment
indicates that it is triggered by the treatment.
A recent study demonstrated that “circulating epithelial cells were
already present before surgery in all patients. During the first 30–60
min after surgery values did not change immediately. They started increasing
during the following 3 to 4 days up to thousand fold in 85% of treated patients
in spite of complete resection of the tumor with tumor free margins in all
patients. “ (4)
Implication for therapy
If tumor and metastasis are indeed one organ (system) tumor reduction
will raise the rate of metastasis. Which supports the approach of this
site. As long as tumor does not impinge upon a vital function and does not
cause pain or suffering it ought to be left intact. Treatment ought to preserve
the tumor and alleviate its secondary manifestations.
Bi-modal hazard rate
(BMH)
The above observations explain
why following breast cancer surgery
the hazard rate rises. Tumor ablation raises
the metastatic rate which accounts for the rising hazard.
Additional reading:
Pernicious cachexia
Metastasis following treatment
Bi-modal hazard rate
WOB
controls cancer
Allometric law and complexity
References
1 ZiMiang Wang et al. The Reconstruction of Kleibers
Law at the Organ-Tissue Level
J. Nutr. 131:2967-2970, November 2001
2 Calder, W. A., III (1984) Size, Function, and Life History
1984 Dover Publications New York. .
3 Romano Demicheli, Elia Biganzoli,
Patrizia Boracchi, Marco Greco, William J.M. Hrushesky, Michael W. Retsky.
Allometric Scaling Law Questions the Traditional Mechanical Model
for Axillary Lymph Node Involvement in Breast Cancer
Journal of Clinical Oncology,
Vol 24, No 27 (September 20), 2006: pp. 4391-4396
4. Oumar Camara, Andreas Kavallaris, Helmut Nöschel,
Matthias Rengsberger, Cornelia Jörke, and Katharina Pachmann
Seeding of epithelial cells into circulation during surgery for breast cancer:
the fate of malignant and benign mobilized cells
World J Surg Oncol. 2006; 4: 67.